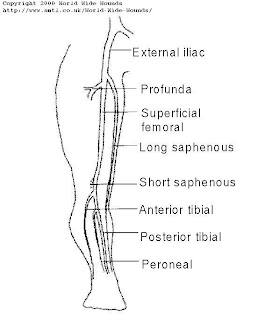
Figure 7: The main arteries of the lower limb.
Figure 7: The main arteries of the lower limb.Patients are normally referred with claudication (pain on walking, particularly uphill) or with ulcers around the ankle and on clinical examination the ankle pulses are likely to be weak or absent. The main options for treatment are either (a) to encourage the patient to exercise and develop collateral vessels to take blood around the site of disease, (b) to perform angioplasty which involves passing a balloon catheter down the artery and inflating it at the sites of narrowing or blockage to dilate the vessel, or (c) to surgically insert an graft to bypass the diseased portion of the vessel [5] . The clinical information required is therefore the site and severity of any narrowing of the vessel and the site and length of any blockages of the main vessels. In the presence of multiple stenoses, the study can indicate which are causing the more critical restrictions to blood flow. The referring clinician can use this information to decide whether intervention is appropriate, and, if so, whether to proceed to angioplasty or to insert a graft [6] .
The examination starts with the patient lying supine with the head slightly raised. Coupling gel is put on the thigh from groin to knee over the path of the artery. The probe is placed on the skin in the groin and the common femoral artery identified using the colour Doppler display. The scanner is switched to duplex mode, and the blood velocity waveform in the common femoral artery is obtained. The waveform is usually biphasic or triphasic. The peak systolic blood velocity normally lies between 90 and 140 cm/s (ref 3, p 260). Values significantly above this may indicate local stenosis, while values below can indicate low flow caused by proximal or distal occlusion. The presence of any plaque intruding into the lumen is noted, and the degree of stenosis is estimated. (Figure 8) shows a scan of a femoral artery with a small protruding plaque causing about 20% stenosis.
 Figure 8: A plaque protruding into the lumen of the common femoral artery. The plaque (PL) is small and is causing about 20% stenosis.
Figure 8: A plaque protruding into the lumen of the common femoral artery. The plaque (PL) is small and is causing about 20% stenosis.The shape of the waveform is important because a monophasic waveform can indicate proximal disease in the iliac vessels. The biphasic or triphasic waveform occurs because the main blood vessels in the leg are elastic and are dilated by the increased pressure during systole. This creates a reservoir of blood which empties during diastole. The volume of blood in the reservoir is more than enough to supply the limb, and the excess flows back up the vessel into the abdominal aorta creating the reverse flow component (Figure 9). An abnormal monophasic waveform without the reverse component occurs when the volume in the reservoir is insufficient and extra flow is required during diastole. This is usually because an iliac stenosis or occlusion reduces the blood available to fill the reservoir during systole, but may also occur when there is a large flow to the limb caused by exercise or gross infection.
Proximal disease can also be indicated by turbulence in the common femoral artery. Turbulence is created in eddies distal to a tight stenosis, and the eddies then travel downstream with the blood flow. They can be detected as spikes in the blood velocity waveform (Figure 10), usually on the downslope at the end of systole. The turbulence is more likely to be created during peak systole when the local blood velocity is highest, but appears later than this distally because the systolic pressure pulse travels faster than the eddying blood. The delay between peak systole and the appearance of the turbulence in the common femoral artery can give an indication of the site of the proximal iliac stenosis. Jager et al [7] have described the shape of the waveform in the lower-limb arteries and the changes associated with different degrees of stenosis.
 Figure 9: Schematic generation of a biphasic waveform. During systole (a), the heart pumps blood into the peripheral vessel and the branches. The peripheral vessel expands. During diastole (b), the vessel contracts. There is more than enough blood in the vessel to supply the periphery, and the excess flows backwards into the more proximal branches. A biphasic waveform is obtained at the point marked with an asterisk.
Figure 9: Schematic generation of a biphasic waveform. During systole (a), the heart pumps blood into the peripheral vessel and the branches. The peripheral vessel expands. During diastole (b), the vessel contracts. There is more than enough blood in the vessel to supply the periphery, and the excess flows backwards into the more proximal branches. A biphasic waveform is obtained at the point marked with an asterisk. Figure 10: Turbulence in the common femoral artery. The blood velocity waveform contains spikes (marked I) just after peak systole. These represent turbulence generated from a proximal tight stenosis
Figure 10: Turbulence in the common femoral artery. The blood velocity waveform contains spikes (marked I) just after peak systole. These represent turbulence generated from a proximal tight stenosis  Figure 11: A superficial femoral artery stenosis. The colour image shows aliasing, a sharp transition from maximum speed away from the probe (light blue) to maximum towards (yellow). The lumen is narrower at the stenosis and the brighter echoes in the near wall show the presence of plaque, which is causing shadowing to the right of the image.
Figure 11: A superficial femoral artery stenosis. The colour image shows aliasing, a sharp transition from maximum speed away from the probe (light blue) to maximum towards (yellow). The lumen is narrower at the stenosis and the brighter echoes in the near wall show the presence of plaque, which is causing shadowing to the right of the image. Figure 12: Velocity waveform through a stenosis. The peak blood velocity through this superficial femoral artery stenosis is greater than 3.9 m/s, compared with 0.26 m/s just proximal to the stenosis. This increase in velocity shows a very tight stenosis.
Figure 12: Velocity waveform through a stenosis. The peak blood velocity through this superficial femoral artery stenosis is greater than 3.9 m/s, compared with 0.26 m/s just proximal to the stenosis. This increase in velocity shows a very tight stenosis. If iliac disease is suspected, either from clinical examination or from a monophasic common femoral waveform, the aorto-iliac segment can be scanned [12] . A 3.5 MHz probe is usually used to give better penetration and a wider field of view. Access to the vessels can be difficult if overlying bowel and bowel gas block the ultrasound. Some centres give an enema before scanning this region, but in thin patients a satisfactory examination is often possible without bowel preparation. The operator is again looking for narrowing or blockage of the artery and the same criteria are used. If distal disease is suspected, some of the small arteries below the knee can be examined. The posterior tibial artery is usually accessible just above the ankle from the medial aspect, and can be traced up the leg as it gets deeper. The artery runs parallel to a pair of veins (Figure 13) and this can aid identification. The operator is again looking for evidence of stenosis or occlusion, but these vessels are small and close to the limit of resolution of all but the most modern scanners, and absence of detected flow may indicate lack of sensitivity of the equipment rather than occlusion.
 Figure 13: Peroneal artery and paired veins. The arterial flow, shown in red, is from left to right with a component towards the probe. The venous flow, shown in blue, is in the opposite direction. The anterior and posterior tibial arteries also lie between paired veins.
Figure 13: Peroneal artery and paired veins. The arterial flow, shown in red, is from left to right with a component towards the probe. The venous flow, shown in blue, is in the opposite direction. The anterior and posterior tibial arteries also lie between paired veins.http://www.blogger.com/www.worldwidewounds.com/.../Doppler-Imaging.html